Digital bone twin by OSORA medical
Fractures in focus: predicting rather than waiting
Bone fractures are generally healed by the body without any issues. However, there are hundreds of thousands of cases each year in which a fracture either fails to heal or only does so slowly. To reduce the number of cases where this happens, a start-up called OSORA medical has developed methods to predict the healing process and, if necessary, make preventative adjustments.
In Germany alone, there are around three million bone fractures per year, meaning this is a significant risk for everyone. Usually, a fracture 'simply' involves dealing with the pain and the reduced mobility that lasts for a few weeks or months before everything is back to normal. However, this is not always the case: in 5 to 10 percent of fractures, a fractured bone fails to heal properly or does not unite over an extended period (referred to as non-union); in an additional 10 to 15 percent of cases, the fracture is slow to heal.1) 2) This often results in multiple surgeries, persistent pain and limitations that can be as debilitating as severe congestive heart failure.3) Not to mention the high socioeconomic cost, as treatment is much more expensive than when fractures heal normally.4)
Personalised predictions of healing processes
 The two founders of OSORA medical GmbH: Dr. Andreas Arnegger (left) and Dr. Frank Niemeyer (right). © OSORA medical
The two founders of OSORA medical GmbH: Dr. Andreas Arnegger (left) and Dr. Frank Niemeyer (right). © OSORA medicalIn general, the self-healing mechanism of bone fractures functions remarkably well. However, it is not infallible: it can be compromised by factors such as excessive movement at the fracture site, insufficient blood supply, large gaps between bone fragments or infections. Additionally, patient-specific factors such as comorbidities, age, gender and the type of fracture also play a role. The treatment approach is also significant: is it conservative or surgical? How is the fracture stabilised and in which position? Numerous influencing factors, all of which have varying degrees of impact on the success of healing.
However, a key challenge remains: how should these parameters be weighted and related to one another, and what implications would this have for treatment decisions? While individual influencing factors are well documented, and various scoring systems – essentially point-based risk assessment tools – are already available, treatment decisions are still largely based on the surgeons’ intuition and experience. "This approach lacks scientific rigour, reproducibility and objectivity," say economist Dr. Andreas Arnegger and human biologist and computer scientist Dr. Frank Niemeyer. As a response to this, they founded OSORA medical GmbH in 2023, an Ulm-based start-up and spin-off from the University of Ulm. The company’s objective is to support more precise and effective treatment strategies by integrating advanced methods from biomechanics, medical imaging, artificial intelligence and digital twin technology that can predict bone fracture healing in individual patients. "We aim to transform medical intuition into something that can be measured and reliably predicted," Arnegger explains. "By complementing established guidelines and clinical experience with simulation-based insights, we seek to enhance decision-making and improve patient outcomes. In other words, supplementing clinical gut feeling with concrete data."
Risk-free testing in the fracture simulator
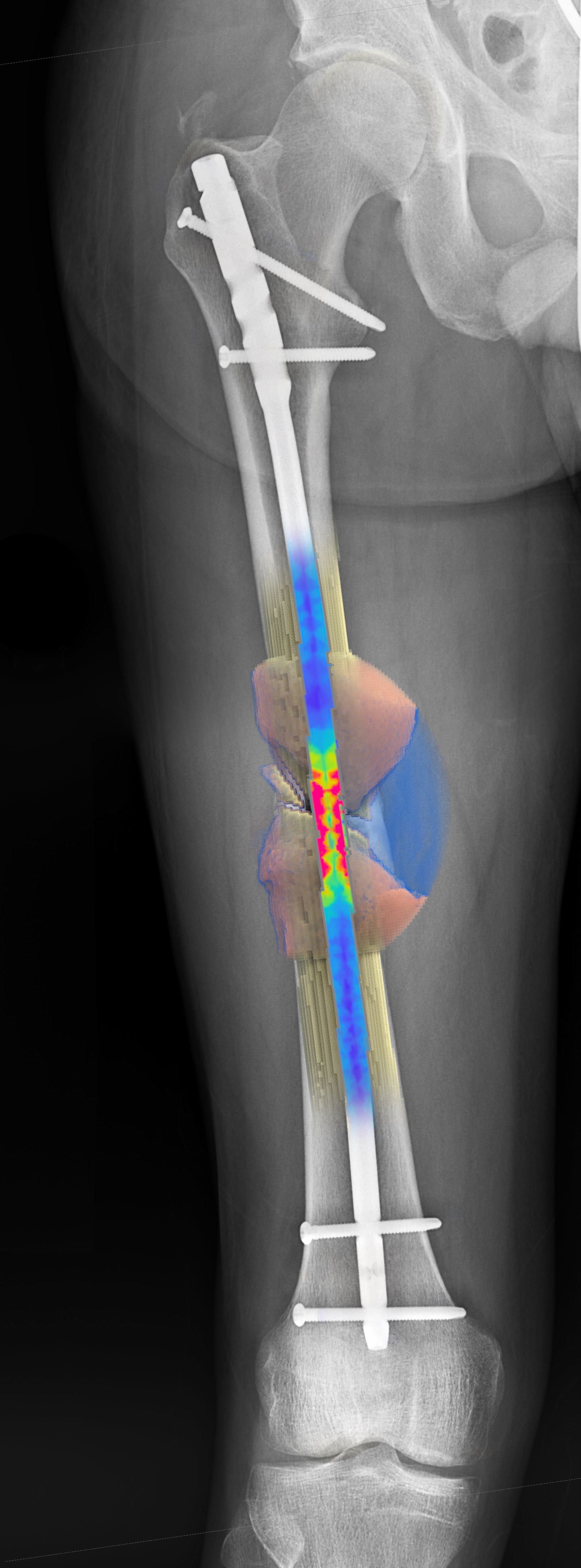 Prediction of bone healing using augmented reality: Patient data and medical images are combined with digital elements to support treatment decisions. The colours represent mechanical load distribution (red = high load on the implant, green = moderate load, blue = low load), while the brown thickening indicates the virtual callus shown by the simulation. It is within this callus that tissue changes occur until complete bone healing is achieved. © OSORA medical
Prediction of bone healing using augmented reality: Patient data and medical images are combined with digital elements to support treatment decisions. The colours represent mechanical load distribution (red = high load on the implant, green = moderate load, blue = low load), while the brown thickening indicates the virtual callus shown by the simulation. It is within this callus that tissue changes occur until complete bone healing is achieved. © OSORA medicalResearchers at the Centre for Scientific Computing (UZWR) at Ulm University have been working on the possibility of simulating bone healing since the late 1990s as part of the 'Ulm Fracture Healing Model' research project – an initiative in which OSORA co-founder Dr. Frank Niemeyer has been actively involved. "The original idea was to simulate different treatment strategies for bone fractures in a low-risk environment – essentially a medical equivalent of a flight simulator," explains Dr. Andreas Arnegger, who, as an avid cyclist, first connected with the research team through his own injury experience. This approach has proven highly effective, as evidenced by numerous publications. The model has not only demonstrated that mechanical forces play a critical role in regulating bone healing and that the process unfolds in distinct biological phases. It has also highlighted the individuality of each fracture, underscoring the need for patient-specific treatment strategies. Today, researchers are able to simulate clinical healing processes, generate individualised prognoses and even predict potential complications.5)
"In addition, there were two key factors that drove us to start the spin-off. Firstly, clinical need – that is, the large number of musculoskeletal injuries that occur every day and are not always treated optimally, simply because there is no objective basis for decision-making. Secondly, the technical foundations were in place: a wealth of clinical data plus the necessary computing power," says Arnegger. Supported by a four-member advisory team specialising in medicine and regulatory affairs, the two founders developed the clinical planning tool OSsitant based on the findings of the UZWR researchers; it is currently in the prototype phase.
Digital twin enables treatment optimisation
OSsistant is designed as a versatile tool for clinicians, implant manufacturers and the next generation of medical professionals. Within a virtual learning environment, students as well as experts in medicine and engineering can explore and better understand the complex interactions between biomechanics and fracture healing – entirely without risk. Arnegger describes the training module as a 'fracture playground.' "It allows users to work through real clinical scenarios and evaluate different treatment options," he explains. "For instance, one can assess whether a thicker nail is more suitable for a femoral fracture, or whether plate fixation may offer advantages. While a nail typically creates a more rigid construct, plate fixation allows for greater initial flexibility, becoming more rigid over time. "The second approach can therefore offer distinct benefits – insights that can be visualised through simulation in a way that closely resembles real-life clinical practice."
Beyond its fracture simulation environment, OSsistant is also designed to predict healing outcomes to be used in clinical application. Using medical images and patient-specific data, the software first generates a digital twin of the injured bone – a detailed three-dimensional model that accurately represents anatomical structure, fracture configuration, fragment geometry and mechanical properties. Clinicians can then incorporate additional parameters, such as implant type, fixation strategy and load conditions, to evaluate different treatment scenarios. Based on these inputs, the software simulates the healing process and provides an evidence-based assessment of whether recovery is likely to proceed as expected or whether complications may arise.
Treatment decisions can then be made on a more robust, evidence-based foundation. At the same time, the software visualises the progression of healing over time, supporting the planning of follow-up care and rehabilitation strategies. "This allows for seamless patient care from the very beginning," adds Dr. Arnegger. "However, our intention is not to provide specific treatment recommendations, but rather to support clinicians and ease their workload by offering a practical tool for everyday clinical use." To ensure clinical relevance, the founders conducted hundreds of in-depth discussions with hospitals and patient groups. These exchanges helped them better understand clinical workflows, identify unmet needs and define areas where their solution could provide meaningful added value.
Engineering case for implants
In another area of application – in-silico testing – manufacturers can virtually evaluate and optimise implants across many patients under a wide range of conditions before clinical use. This approach simulates long-term healing processes, mechanical load and force distributions, allowing potential mechanical failures to be identified at an early stage. By integrating these insights into the development process, critical biomechanical factors can be addressed prior to clinical testing. "In the automotive industry, such simulation-based engineering approaches have long been standard practice," explains the business development manager. "For our first industrial partners, we have already analysed key mechanical questions – for example, how long a screw needs to be to support optimal healing or how many screws are required." The team is currently extending this work to new fields of application. In collaboration with Ulm University of Applied Sciences, they are investigating various potential applications including the osseointegration behaviour of dental implant systems.
The technology has already demonstrated its value in clinical studies. In collaboration with four BG clinics (ed. note: a BG clinic is a highly specialised trauma and rehabilitation hospital focused on occupational injuries and insurance-funded medical care within the German social insurance system), the start-up has shown how the OSORA platform performs when used by clinicians of varying levels of experience. The findings have already been presented at several conferences. The team is now focused on translating its simulation technology into routine clinical practice as quickly as possible. "We are currently working through the regulatory requirements and anticipate market entry around 2028/29. If we can possibly achieve this sooner, we will," says Arnegger.