AaviGen GmbH: Hope for heart failure
Gene therapy for weakened hearts
Treating a weak heart – for example after a heart attack – at the GP’s surgery with a single intravenous injection, and without causing serious side effects: what sounds almost too good to be true is actually already under development. The Heidelberg-based biotech company AaviGen is working on a platform technology based on adeno-associated viruses that can help introduce therapeutic genes in a highly specific way into diseased heart muscle cells where they can exert their healing effect.
A healthy heart keeps our body supplied with sufficient oxygen to perform its tasks – and helps us feel fit and efficient. However, if this central organ is only able to perform its tasks to a limited degree, this is then referred to as heart failure. The reasons for this occurring vary and can result from years of high blood pressure or a heart attack, for example. Weak heart pumping affects several million people in Germany alone, where the numbers affected are on the increase, as is the case in all other industrialised countries.1)
Once heart failure is diagnosed, the 5-year survival rate is only about 50 percent, because current treatment options are extremely limited: the only causal therapy is a heart transplant, which is an option for less than 0.001 percent of patients. For everyone else, the only possibility is to treat the symptoms.2)
Interdisciplinary team of gene therapy pioneers and start-up experts
 Prof. Dr. Patrick Most co-founded AaviGen – a young biotech company that develops curative gene therapies for cardiovascular diseases. © AaviGen
Prof. Dr. Patrick Most co-founded AaviGen – a young biotech company that develops curative gene therapies for cardiovascular diseases. © AaviGenNow there is hope in sight: the biotech company AaviGen GmbH from Heidelberg is developing tiny, heart-specific, synthetic viral ‘universal taxis’ that could specifically deliver therapeutic genes to the site of action and support or heal heart cells. The start-up can draw on many years of expertise in the development of curative gene therapies for cardiovascular diseases: Prof. Dr. Patrick Most, one of the company's founders and its CEO as well as head of the Molecular and Translational Cardiology Section at the Department of Cardiology at Heidelberg University Hospital, has been doing research in this field for a long time. Back in 2014, he founded InoCard GmbH together with Prof. Dr. Hugo Katus. With its first-generation gene therapy for heart muscle weakness, InoCard became part of the Dutch gene therapy specialist uniQure.
In addition to Most, the management team of AaviGen comprises three other co-founders: Prof. Dr. Hugo Katus, CMO and leading international expert in cardiovascular medicine thanks to his many years as medical director of the Department of Cardiology at Heidelberg University Hospital, Prof. Dr. Marc Lerchenmüller, CFO and financial economist specialising in healthcare after many years of experience at the Boston Consulting Group New York, and Dr. Martin Busch, COO and, as a biotechnology expert, responsible for production processes, among other things. The young company is currently being financed through an investment by Dietmar Hopp.
Heart-specific recombinant AAVs as universal taxis to the heart
"While the principle of gene therapy was developed decades ago in academia and the enormous therapeutic potential has already been documented through the successful approval of gene therapy drugs in the USA and Europe, nothing has yet reached the clinic for heart patients," Most explains. "The reason for this is not that there are no therapeutic genes that could cure diseases of the heart muscle, but that it has not yet been possible to get them to the target site in effective doses and simple forms. Our goal is to fundamentally change this in order to benefit patients. With the technological AaviGen platform, we are developing synthetic gene shuttles to help transport and place therapeutic genes into the diseased heart muscle in a personalised, safe, simple and precise manner. Specifically, we are currently focusing on developing gene therapies for acquired or congenital, i.e. genetically determined, cardiovascular and cardiopulmonary diseases."
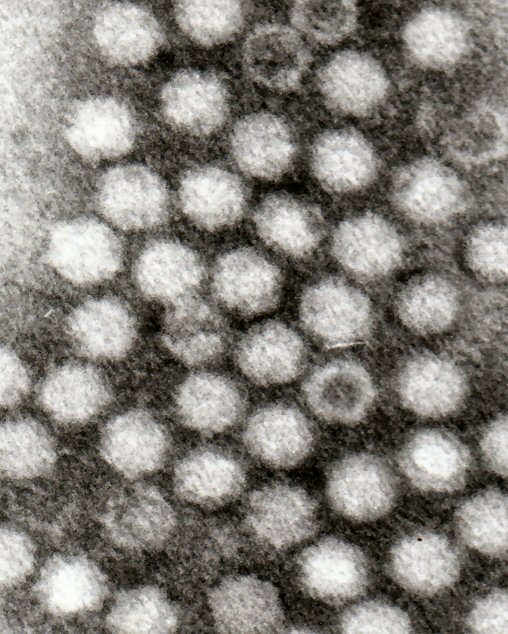 AaviGen uses adeno-associated viruses (AAVs) as gene shuttles for transporting the therapeutic sequences to the heart. Source: Dr Graham Beards, Wikipedia, CC BY-SA 3.0, https://creativecommons.org/licenses/by-sa/3.0/deed.en
AaviGen uses adeno-associated viruses (AAVs) as gene shuttles for transporting the therapeutic sequences to the heart. Source: Dr Graham Beards, Wikipedia, CC BY-SA 3.0, https://creativecommons.org/licenses/by-sa/3.0/deed.enThe expert expects the first product to be tested in a clinical trial in around six to seven years’ time: "We are at the start of what will be a challenging task, but we can already see from the international competition around us that we are correctly positioned with our unique selling propositions. Among other things, there is a lot of interest in our work from large biopharmaceutical companies."
AaviGen uses recombinant adeno-associated viruses (AAVs) as delivery vehicles to bring therapeutic genes (inside the AAV capsid) to the diseased heart. The research team develops synthetic varieties of these AAVs using biotechnological processes: "We modify the AAV surfaces genetically and molecularly in such a way that they ultimately exhibit a high cardiac tropism [editor's note: viral tropism refers to the ability of a virus to infect a certain cell type and multiply] and can thus precisely and reliably introduce the therapeutic gene cassettes into heart muscle cells," Most explains. "This will eventually make it possible to carry out treatments at every GP’s surgery. We envisage just one single intravenous injection, with an effect that can last for several years – or maybe even a lifetime.
The exclusive cardiac vector tropism also has a second key characteristic: because the gene shuttles only target heart muscle cells and bypass the liver, for example, which is the most likely trigger of undesirable effects from gene therapies, it will be possible to dose our gene therapeutics much lower, meaning of course there will be fewer side effects. This radically simplifies the whole system."
Info box: Adeno-associated viruses (AAV)
AAVs are a type of virus that require a helper - an adenovirus - that infects the same cell. They are often used as viral vectors for gene therapies because they are not disease vectors, but are more stable than adenoviruses alone and infect certain cell types just as specifically. However, their relatively small genome is a disadvantage for this application.
AaviGen takes certain naturally occurring AAV variants and creates synthetic variants that, after injection, bring the therapeutic genes only to the heart, rather than also targeting the liver, as is the case with other drugs. This specificity means that the dose can be kept low. And since the AAVs can no longer develop toxicity in the liver, no significant side effects are expected.
The disadvantage of the limited genome available for packaging the therapeutic sequences is either accepted and thus the target kept small enough to fit into the AAV capsid. This is then referred to as gene addition – i.e. the presence of an extra copy number of certain gene sequences in the heart muscle. Or, if this is not possible, the mini-CRISPR/Cas method can be used, in which the therapeutic gene cassettes are packaged using gene editing.
Gene therapy strengthens the remaining healthy heart muscle cells
Once in the heart muscle cells, the therapeutic genes are released and expressed. In the case of post-infarction myocardial weakness, for example, the effect is that the remaining, functional residual muscle is strengthened by the gene therapy, which compensates for the loss of heart tissue resulting from disease.
Ultimately, the Heidelberg researchers are planning a portfolio of several AAV capsids, all specific for cardiac muscle cells but targeting different heart diseases and enabling personalised therapies: "Depending on the requirements of the therapeutic gene or the indication, a cardiac AAV vector with the appropriate properties can be selected," says the professor. Libraries of billions of sequence variants are currently being tested. Another innovation: normally, such developments are started in cells. However, this only rarely works in animal models, which are required by the health authorities when developing gene therapies. "We turn this process around and develop directly in the appropriate animal models required for demonstrating the safety and effect of therapies in humans," says Most.
But it is not only the ability to reach the heart that determines the suitability of a virus variant. "It must also be easy to produce in order to be able to treat the highest possible number of heart patients," emphasises the physician. "We have learned from previous projects how important it is to address this at an early stage. That is why we are already working with manufacturers of AAV-based gene therapeutics to prepare the complex production processes. It goes without saying that we have to be in close contact with the regulatory authorities in order to make sure a chosen variant is safe." These viruses can no longer reproduce on their own – in either body cells or in nature – because they are recombinant and this ability has been taken away from them.
Baden-Württemberg government and university as godfathers of the start-up
In addition to Dietmar Hopp's total commitment, the support of the University of Heidelberg was also decisive for the young company. "In particular, Prof. Eitel, the university’s rector, was already convinced with our first start-up that it is possible to successfully bring academic innovations into bioindustrial translation and thus ultimately to the patient," says Most. "And by providing the necessary employment models, among a number of other things, he has done a great deal to promote the innovative concept of academic intrapreneurship at Heidelberg University." And Most also particularly emphasises the support of the Baden-Württemberg government: "Baden-Württemberg has been the godfather for our company, so to speak, because its translation programmes within the framework of the Forum Health Region Baden-Württemberg made a very significant contribution to our decision to found AaviGen."