rMSI technology
New multispectral imaging technology improves endoscopic tumour detection capabilities
The quality of minimally invasive surgery depends to a large extent on the imaging properties of the endoscopes used. The Mannheim-based company Thericon GmbH has developed a multispectral imaging technology that overlays views from multiple light channels in real time to create a detailed image on which tumours can be better identified.
Back in Antiquity, human body cavities and passages were examined with the aid of a mirror (speculum) to detect diseases. However, ensuring enough light in the body cavity for the observer to see the image of the interior was a constant problem. The first person to successfully achieve this was the Frankfurt physician Philipp Bozzini, who in 1806 published a report on the light conductor he had constructed and thus established endoscopy (from the ancient Greek endon = inside and skopein = to look at). The instrument he used consisted of two separate chambers: one that guided the light generated by a candle into the interior of the body with the aid of a concave mirror, and the other that reflected the image into the eye of the observer. This principle of separate channels for light and image transport and an external light source has been retained in modern endoscopes.
Minimally invasive surgery for bladder cancer
From the very beginning, endoscopy was used for examining the urethra and bladder (cystoscopy). Today, in combination with fine surgical instruments, endoscopy is routinely used for the minimally invasive removal of tumours in the bladder. Bladder cancer is one of the most common cancers worldwide and has a very high recurrence rate of nearly 65 percent. One of the most important reasons for the high recurrence rate of bladder cancer is incomplete removal of the original tumour as a result of malignant tissue often being difficult to identify.
Standard endoscopic examination uses white light (WL), which is specifically suitable for identifying papillary tumours (tumours that grow from tissue that lines the inside of an organ), but has weaknesses when it comes to identifying flat or very small tumours. For this reason, additional imaging technologies are now being used: photodynamic diagnostics (PDD), in which tumour cells glow red when exposed to blue light after a fluorescent contrast agent is administered to make them easily identifiable. Unfortunately, however, under these conditions the field of view is too dark for surgery, making it necessary to switch back to WL mode. In addition, false-positive findings occur quite frequently. Narrow band imaging (NBI), which uses only blue and green light, can be used to enhance the contrast of the mucosal surface, as blood vessels appear dark due to the fact that haemoglobin is an effective light absorber in this light wavelength range (enhanced vascular contrast, EVC).
New multispectral imaging in real time
Dr. Nikolaos Deliolanis has been working in the field of biomedical optics with a particular focus on multispectral imaging since 2008; first at Helmholtz Zentrum München and since 2012 at the Fraunhofer Project Group for Automation in Medicine and Biotechnology (PAMB) in Mannheim. The physicist and his team have developed an imaging method for minimally invasive surgery that significantly improves tumour identification. "We overlay different images to create a multi-parametric view so that surgeons can see all of the tissue’s anatomical and functional information in one image," explains Deliolanis. Specifically, this means that white light images can be combined with PDD images and EVC views, and information from additional fluorescence images can be integrated. This compensates for the weaknesses of the individual imaging modes, and produces a detailed image with clearly identifiable tumour boundaries.
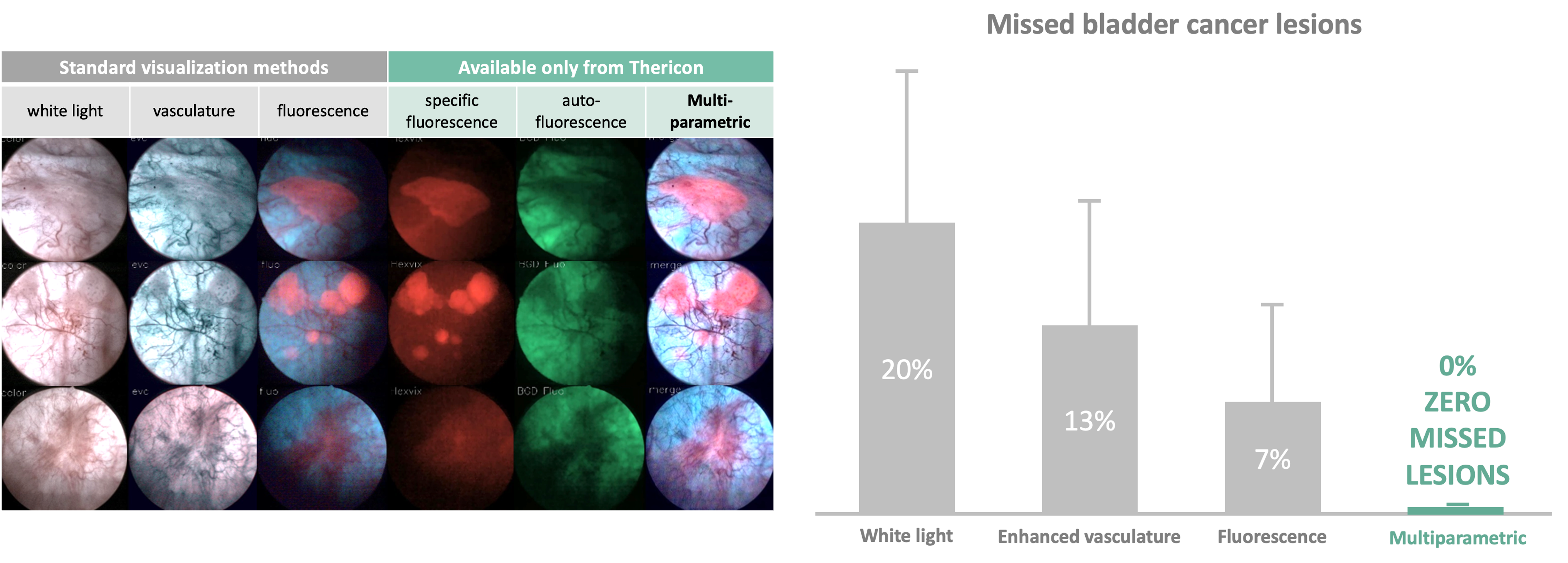 Endoscopic visualisation of different tissue lesions with different visualisation methods (left). Thericon's rMSI (real-time multispectral imaging) technology provides a differentiated image and best detection of the red fluorescent tumour. Proportion of missed tumour lesions with the different visualisation methods (right). © Thericon GmbH
Endoscopic visualisation of different tissue lesions with different visualisation methods (left). Thericon's rMSI (real-time multispectral imaging) technology provides a differentiated image and best detection of the red fluorescent tumour. Proportion of missed tumour lesions with the different visualisation methods (right). © Thericon GmbHWhat makes this possible is a multispectral LED light source that generates different coloured light pulses at short time intervals that excite different fluorescences in the tissue. The emitted light is detected in the camera head of the endoscope via built-in filters and sensors, processed in a control unit and assembled in real time to form an image that can then be transmitted to a monitor. The patented rMSI (real-time multispectral imaging) technology makes surgeons' work much easier, as rather than having to switch between the different views, they now receive all the information simultaneously in one image.
Thericon wants to bring rMSI process to market maturity
However, there is still a long way to go before the technology is ready for the market. Proof of concept for the technology was provided as part of the BMBF's GO-Bio funding programme, and an initial pilot study was conducted with bladder cancer patients. This pilot study was conducted in cooperation with the Department of Urology and Urosurgery at Mannheim University Hospital under the direction of Prof. Dr. Christian Bolenz and Prof. Dr. Maximilian Kriegmair. The scientists compared the rMSI technology with existing detection methods and were able to show that up to 20 percent of tumours were missed with conventional systems, whereas all tumours could be detected with rMSI. This work was recognised by the European Society of Urology with the 2019 Vision Award for the most innovative study.
 Dr. Nikolaos Deliolanis founded Thericon GmbH in 2019 together with Dr. Bartłomiej Grychtol and Dr. Steffen Schabel to bring the rMSI technology to market. © University of Heidelberg / Schatral
Dr. Nikolaos Deliolanis founded Thericon GmbH in 2019 together with Dr. Bartłomiej Grychtol and Dr. Steffen Schabel to bring the rMSI technology to market. © University of Heidelberg / SchatralIn the same year, Deliolanis founded Thericon GmbH together with image processing specialist Dr. Bartłomiej Grychtol and marketing and sales expert Dr. Steffen Schabel to further develop the device for the market.
So far, a demonstration prototype made of modified commercially available components has been constructed. In the next few years, a final product prototype will be created and certified so that larger-scale clinical trials can subsequently be conducted. "We want to show not only that our technology is safe and effective, but that it is better than the current standard," Deliolanis explains. "Bladder cancer is just one potential application. The device can be used in many areas of minimally invasive surgery because it generally allows visualisation of different tissue components (e.g., nerves, blood vessels, cancer cells) in real time using contrast agents." Thericon recently received the Mannheim founder award MEXI 2021 in the technology category for its innovative imaging system.
Great future potential
rMSI technology has the potential to fundamentally improve endoscopic imaging. The high reliability and diagnostic sensitivity not only directly benefit patients and surgeons, but can also mean enormous cost savings for the healthcare system due to fewer follow-up operations. The excellent quality of the data generated also enables AI-based algorithms to be learned, thus opening up new perspectives for use in robot-assisted surgery.