Lab-on-a-chip
Microfluidic platform for the best possible cancer therapy
Every tumour and every patient is different, and there are individual reactions to drugs as well as the problem of resistance. Patient-specific cancer treatments require innovative and cost-effective approaches. The TheraMe! consortium has developed a novel instrument: a combination of microfluidic experiments and mathematical modelling for use in cancer precision medicine to prevent incorrect therapy options.
As the number of cancers increases, intensive research is being carried out into ways of better understanding how tumours develop and spread and how to combat them. The crux of the matter is that there are no standardised cancers, making effective treatment difficult. Every patient, and therefore every tumour, is different, and the response to medication therefore differs from one individual to another. This is why the focus is shifting to innovative procedures that make it possible to determine the best possible therapy for each individual patient.
Over the years, many approaches to personalised medicine have been developed, but only a few have made it into clinical routine. The reasons are the high requirements of personalised approaches, namely, that they should be implementable within hours or days so that the therapy can be adapted in a timely manner. At the same time, the therapy should be affordable in comparison to conventional treatments with only inconsequential additional costs. In addition, only small sample quantities of patient material should be required for diagnostic tests. TheraMe! offers a solution for all of this: with the help of microfluidic technology, sample volumes can be reduced to one microlitre, i.e. one millionth of a litre. Small patient biopsies therefore provide sufficient material for extensive test series. The international TheraMe! consortium founded in Heidelberg with the participation of the European Molecular Biology Laboratory (EMBL) has a comprehensive patent portfolio and plans to establish a biotech start-up that will make diagnostic procedures and instruments for personalised cancer therapy commercially available. This project is receiving funding of around 820,000 euros from the German Federal Ministry of Economics and Energy’s EXIST funding programme . Given the expertise behind the project, the granted funds do not come as a surprise: the consortium draws on interdisciplinary expertise in microfluidics (Merten working group), bioinformatics (Saez-Rodriguez working group), clinical oncology (Cramer working group), as well as experts in the fields of physics, biomedicine and business.
 The research groups of Prof. Dr. Christoph Merten (left), Prof. Dr. Julio Saez-Rodriguez (centre) and Prof. Dr. Thorsten Cramer (right) have joined forces to form the TheraMe! consortium to break new ground in personalised cancer therapy.
© TheraMe!
The research groups of Prof. Dr. Christoph Merten (left), Prof. Dr. Julio Saez-Rodriguez (centre) and Prof. Dr. Thorsten Cramer (right) have joined forces to form the TheraMe! consortium to break new ground in personalised cancer therapy.
© TheraMe!
Miniaturised drug screening
The way analyses are currently done means that the cell count obtained from solid tumours is too low to perform extensive tests directly on the tumour. This is where microfluidics offers enormous potential: the miniaturised design, means that thousands of tests can be performed on each biopsy. In the process, the patient's tumour cells are exposed to a combination of drugs. Twenty-four hours are sufficient to determine which of the combinations kills the tumour cells most efficiently. "We wanted to create a platform that would allow us to quickly and cost-effectively determine the best tumour therapy for each individual patient at any given time, even in cases where resistance has developed," explains Prof. Christoph Merten, head of the Biomedical Microfluidics Research Group at the Swiss Federal Institute of Technology in Lausanne (EPFL) and an associate scientist at the Ludwig Institute for Cancer Research (LICR) in Lausanne.
For more than 15 years, Merten has been working with over 30 scientists on microfluidic approaches as part of his research in England (MRC-LMB in Cambridge), France (ISIS in Strasbourg), Germany (EMBL in Heidelberg) and Switzerland (EPFL in Lausanne). "Together with our partners, Prof. Dr. Saez-Rodriguez, Prof. Dr. Cramer and Prof. Dr. Eduati, we want to further advance personalised precision medicine for cancer therapy and make it commercially available through a start-up."
Geno- and phenotypic analyses instead of "one size fits all"
The high degree of automation enables complex model studies to be undertaken. "In disease modelling, it is important to take into account both phenotypic and genotypic characteristics," says Merten. One size fits all, as we well know from a population-wide flu vaccination, for example, offers no solution here. "Microfluidically controlled personalised therapy approaches, on the other hand, integrate data from a wide range of tests and the individual patient history in order to determine the optimal treatment for each patient."
TheraMe! extracts a sufficient number of cancer cells both directly from tumour biopsies and from resected tumours, i.e. from the site of the primary tumour. Cultivation steps that cause distortion are thus avoided. "By using direct patient samples, we can deal more effectively with tumour heterogeneity," explains Merten. "We can use our assays to evaluate the efficacy of drugs even before they are administered to patients," he says. Such phenotypic characteristics are important because every patient reacts differently to drugs. In the future, tests will also be carried out at the genetic level. This will assist in the discovery of new biomarkers that can help predict the efficacy of different drugs in each individual patient. In addition, these tests will yield up to a thousand times more data points per patient and per drug tested, making it more accurate to find the best possible therapy option.
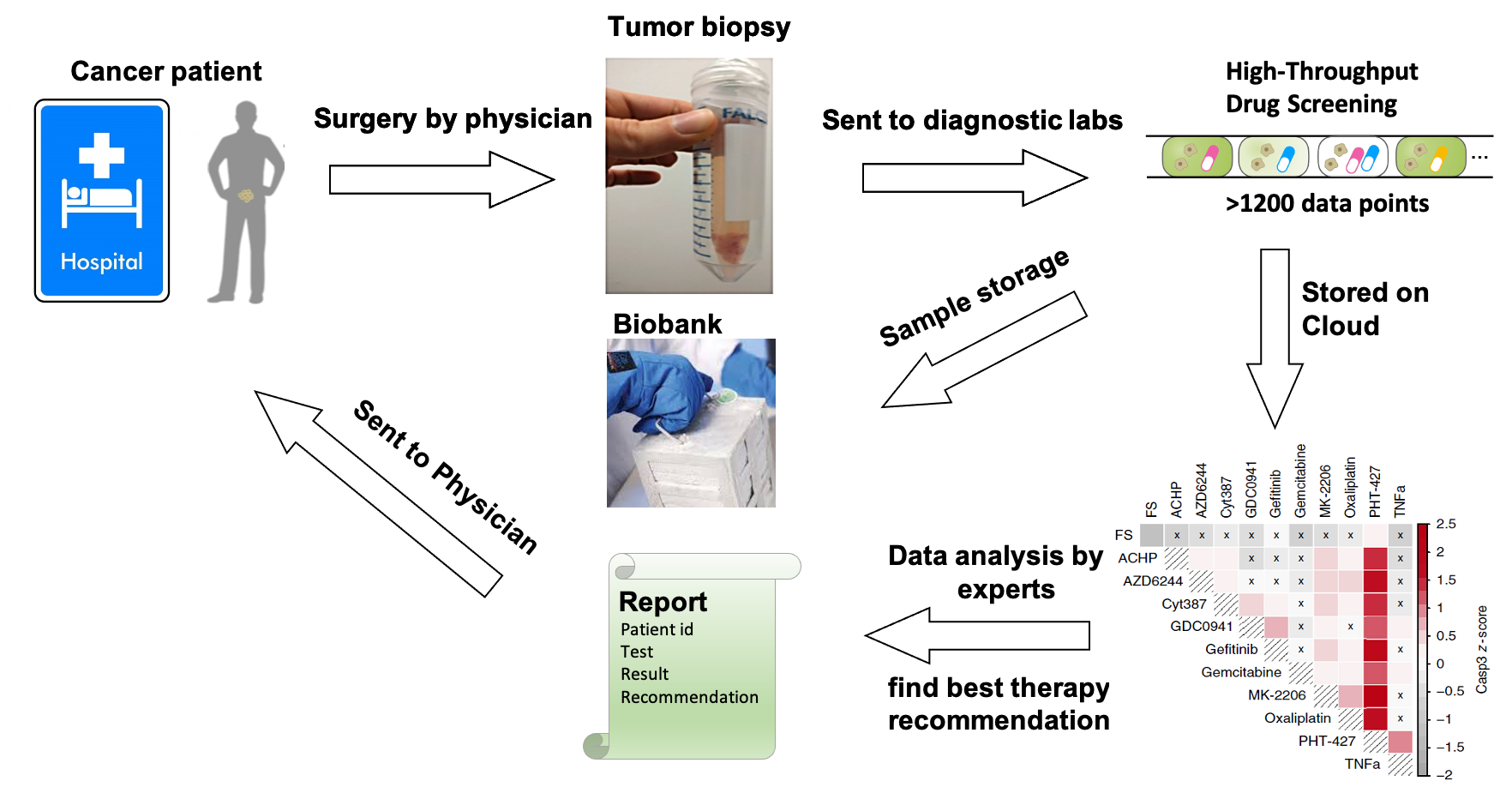 TheraMe! workflow for making the best possible therapy recommendation for individual patients. © TheraMe!
TheraMe! workflow for making the best possible therapy recommendation for individual patients. © TheraMe!The TheraMe! approach far surpasses currently established methods, as Merten explains: "The majority of today's methods use sequencing to detect known biomarkers and derive probabilities of therapeutic success for a few options. However, these methods do not test how much the entire transcriptome and thus also the cancer-relevant signalling pathways change for up to hundreds of therapy options. Furthermore, our analysis of the signalling pathways, even independently of the few known biomarkers to date, allows us to determine the best possible therapy option for each individual patient.”
Small droplets with high output - microfluidics as a future routine tool
Instead of using conventional test tubes or microtitre plates, which require more cells than can be taken from a patient, TheraMe! performs drug testing in microscopically small droplets.
 High precision manufacture of a microfluidic chip using the latest 3D printing technology. Cancer cells, drugs, reagents and oil are injected into channels less than a tenth of a millimetre in diameter to produce microscopic measuring vessels in the form of aqueous drops in an oil phase. This type of miniaturisation allows significantly more tests to be performed on patient cells than before. © TheraMe!
High precision manufacture of a microfluidic chip using the latest 3D printing technology. Cancer cells, drugs, reagents and oil are injected into channels less than a tenth of a millimetre in diameter to produce microscopic measuring vessels in the form of aqueous drops in an oil phase. This type of miniaturisation allows significantly more tests to be performed on patient cells than before. © TheraMe!This approach has many advantages over existing technologies. For example, alongside the response to individual drugs, hundreds of treatment options are tested and displayed on a single screen "as is" rather than as probabilities. Data on the wide range of drug tests is therefore made available before therapy even begins, making it unnecessary for patients to undergo therapies with copious side effects that later prove inefficient. Merten's team can point to remarkable developments: "The results are available within 24 hours of obtaining a very small biopsy sample, at a considerably lower cost than standard diagnostic procedures such as MRI scans. Our system makes it possible to determine the best therapy options directly from patients’ tumour samples. We have been able to validate our approach in mice and successfully demonstrate the procedure on biopsies of tumour patients."
The core technology of TheraMe! is already protected by a US patent, with two patents for additional technologies pending. Since 2017, Merten has also been involved on the scientific side in founding another start-up company that successfully uses microfluidic technology for antibody development – other prospects even include immuno-oncology. Changing the approach from conventional test tubes to microscopically small drops opens up a wide range of possibilities for novel therapies and drugs.
This might also interest you ...